2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure
The format of the previous 2016 ESC HF Guidelines was revised to make each phenotype of HF stand alone in terms of its diagnosis and management. The therapy recommendations mention the treatment effect supported by the class and level of evidence and are presented in tables. In this guideline, we have decided to focus on the diagnosis and treatment of HF, not on its prevention.
The 2023 Focused Update of these Guidelines is available.
Copyright permission
Guidelines and related materials are for use by individuals for personal or educational purposes. No commercial use is allowed. Re-use permission must be correctly obtained from the publisher ESC Guidelines are protected by copyright. As per opt out option under Article 4 §3 of EU Directive 2019/790, the ESC reserves all rights to license uses of ESC Guidelines to train or develop generative artificial intelligence (AI) models, large language models or other deep learning or machine learning models. Any use of ESC Guidelines in software tools, generative AI models, computational models, or algorithms in which ESC Guideline content is included, cited, or transformed in any way requires a formal license agreement.
ESC Chat - Your Guidelines Companion
ESC Chat provides instant and personalised answers to clinical queries, based exclusively on current ESC Clinical Practice Guidelines.
Educational Material

Most recent updates for treating heart failure. ESC 2023 Clinical Practice Guidelines - Webinar Series

Advanced heart failure therapy in HF patients with preserved and mildly reduced ejection fraction
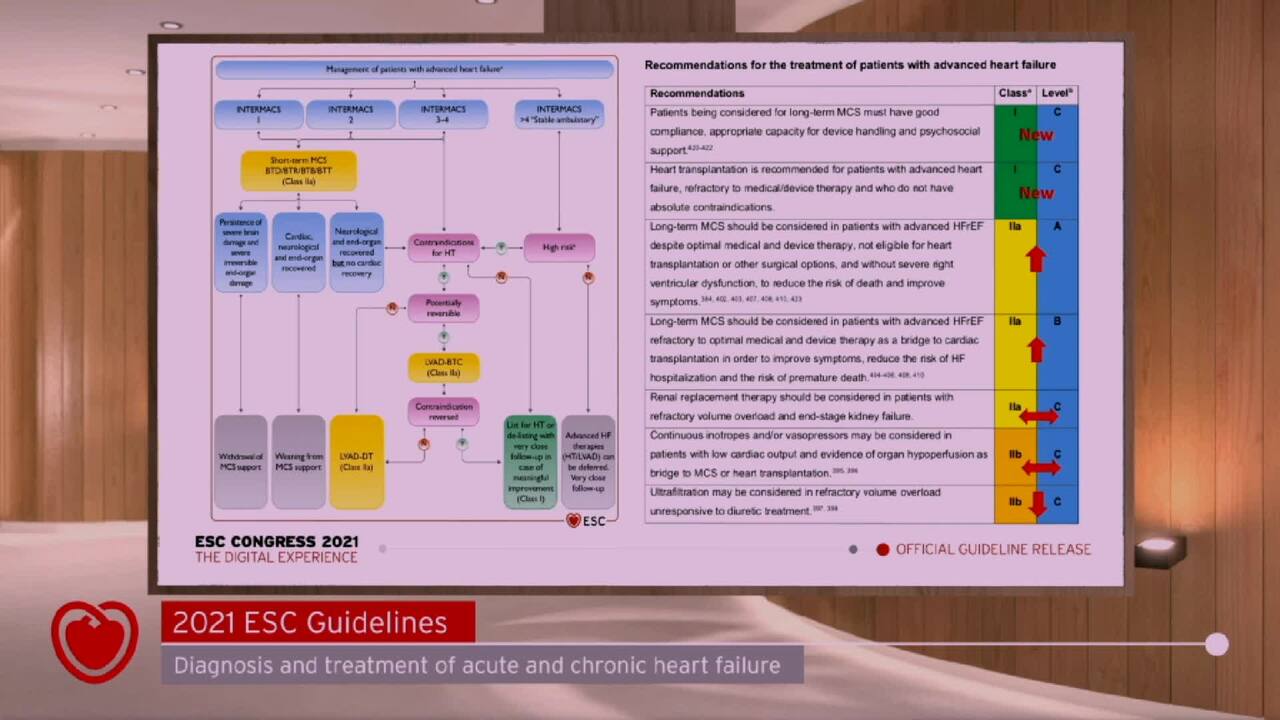
2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure
Tools
Slide set
Educational material
Patient versions of ESC Guidelines
ESC Patient Guidelines translate expert clinical recommendations into clear, everyday language.
ESC Pocket Guidelines Mobile App
Convenient resources available directly on your mobile device.



















































































