2018 Guidelines for Diagnosis/Management of Syncope
While the full text gives formal, evidence-based recommendations according to the standard rules of the ESC, the new supplementary data allow expansion of the content into practical issues, filling the gap between the best available scientific evidence and the need for dissemination of these concepts into clinical practice. ('We have the knowledge: we need to teach it'.)
Copyright permission
Guidelines and related materials are for use by individuals for personal or educational purposes. No commercial use is allowed. Re-use permission must be correctly obtained from the publisher ESC Guidelines are protected by copyright. As per opt out option under Article 4 §3 of EU Directive 2019/790, the ESC reserves all rights to license uses of ESC Guidelines to train or develop generative artificial intelligence (AI) models, large language models or other deep learning or machine learning models. Any use of ESC Guidelines in software tools, generative AI models, computational models, or algorithms in which ESC Guideline content is included, cited, or transformed in any way requires a formal license agreement.
ESC Chat - Your Guidelines Companion
ESC Chat provides instant and personalised answers to clinical queries, based exclusively on current ESC Clinical Practice Guidelines.
Educational material
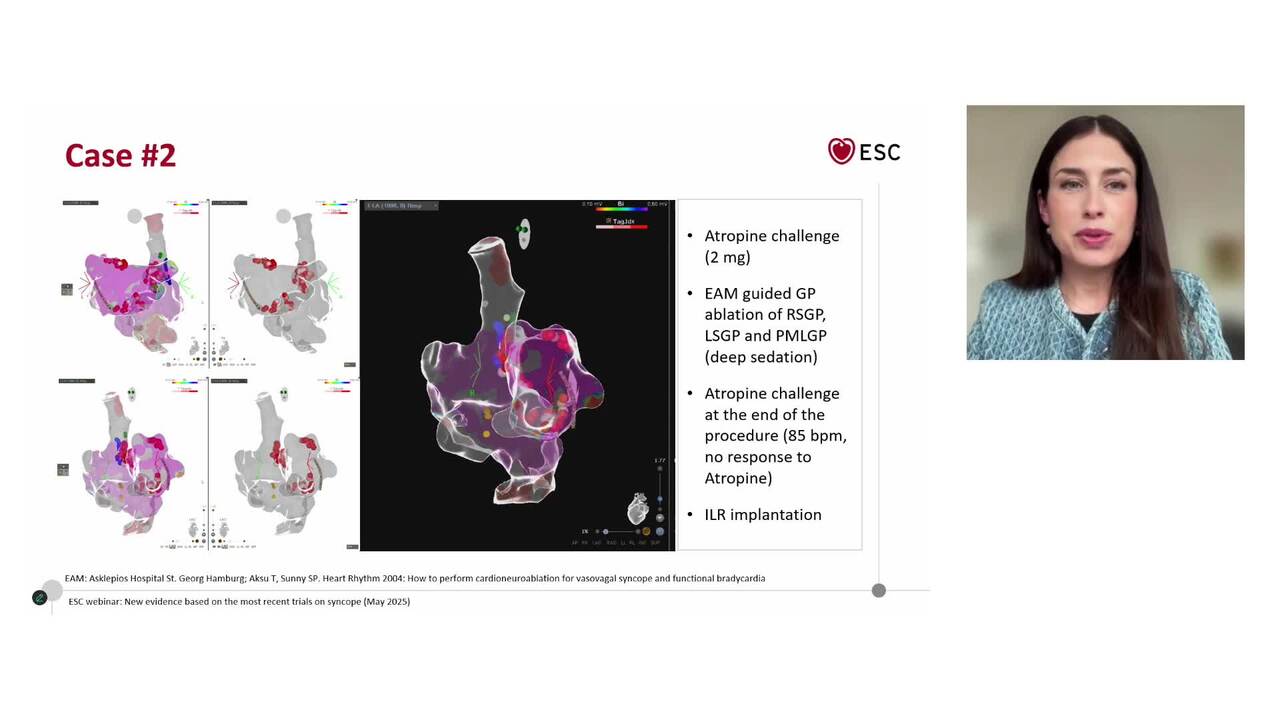
New evidence based on the most recent trials on syncope
Diagnosis and management of non-cardiac syncope: a 2025 update
2018 ESC Guidelines on Syncope
Tools
Slide Set
Educational material.
Patient versions of ESC Guidelines
ESC Patient Guidelines translate expert clinical recommendations into clear, everyday language.
ESC Pocket Guidelines Mobile App
Convenient resources available directly on your mobile device.
Task Force members


























































