Genetic consultation in cardiomyopathies
March 2026

Webinars

Principles of genetic testing and variant interpretation in cardiomyopathies

Genetic consultation in cardiomyopathies : from test to clinical decision-making
Essentials
ESC Guidelines
2023 ESC Guidelines for the Management of Cardiomyopathies
Genetic testing in dilated and non-dilated cardiomyopathy
When to suspect a genetic cardiomyopathy
How can genetics aid cardiovascular risk management in diabetes?
How should genetics inform the treatment of hypertrophic cardiomyopathies?

Relevant textbook chapters

Exclusively for members
Dig Deeper
In practice

How to read and interpret a genetic testing report in inherited cardiovascular conditions
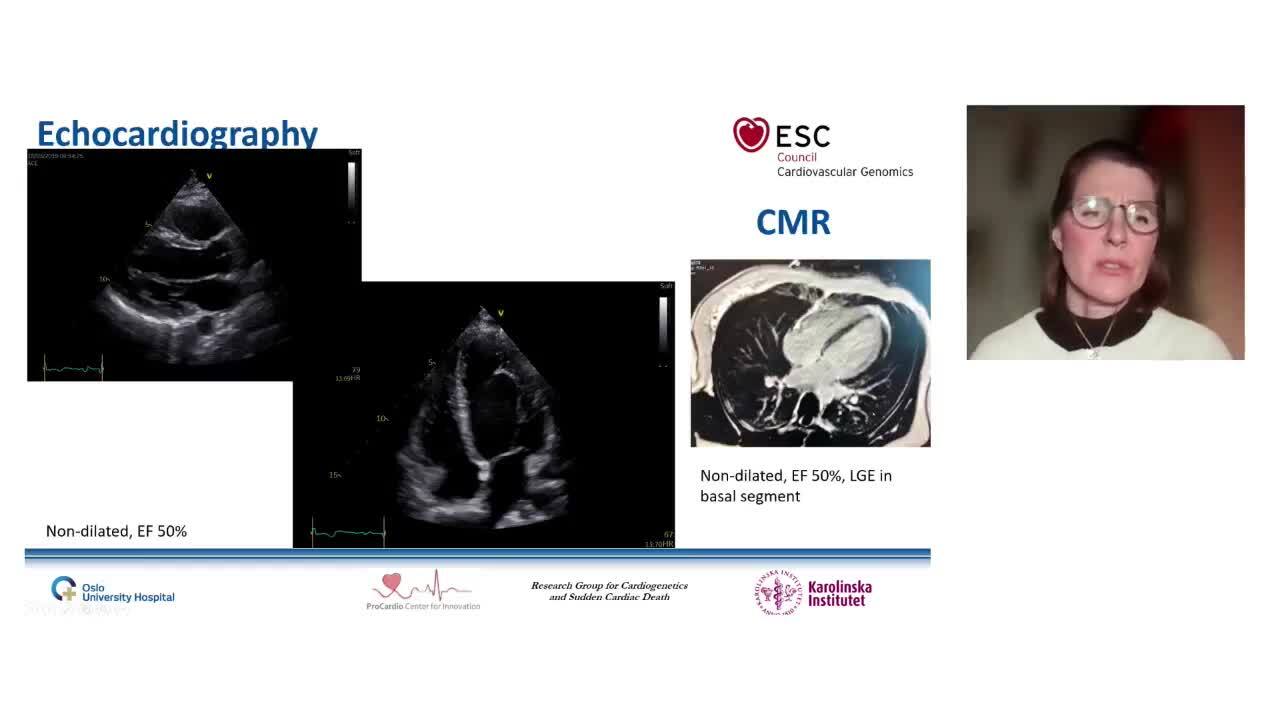
Preimplantation genetic diagnosis and pregnancy in inherited cardiovascular disease

Primary electrical disorders: between ECG and genes
Interface with the specialists

Cardiovascular genetics in practice: what to know for today and tomorrow
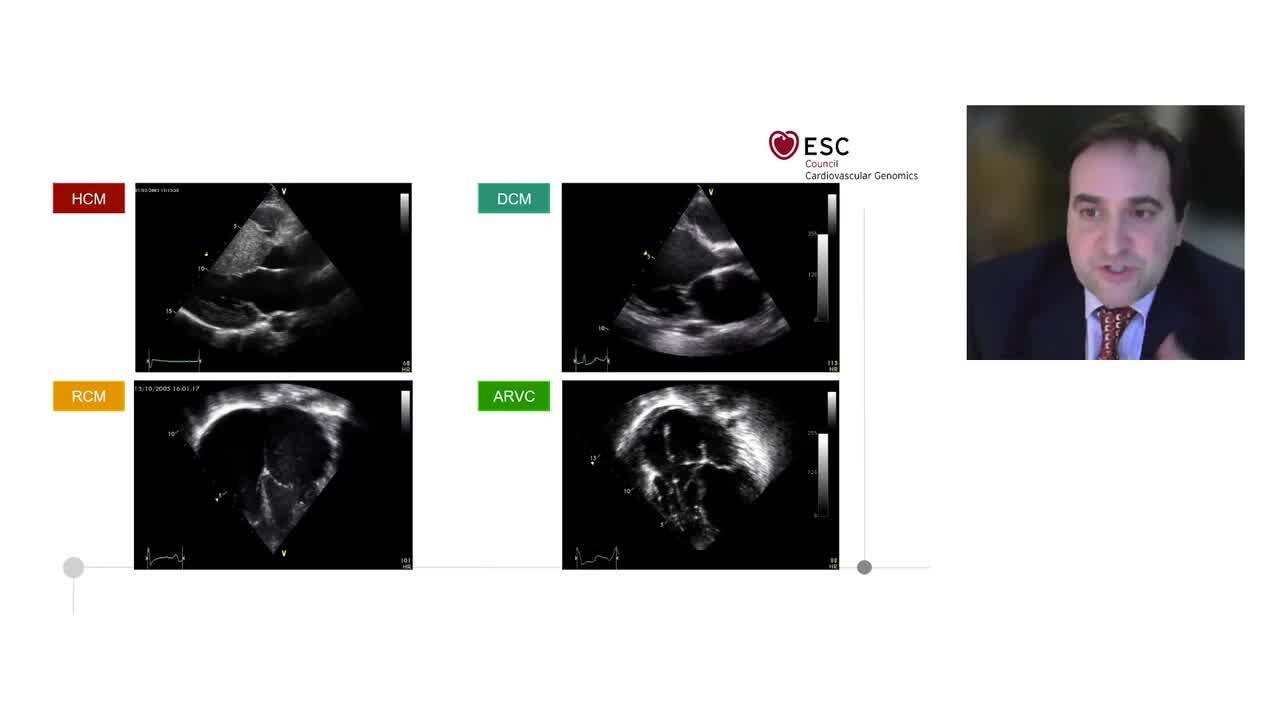
Interpretation and actionability of genetic variants in cardiomyopathies
Inherited cardiomyopathies: clinical and genetic updates
Pioneers' viewpoint
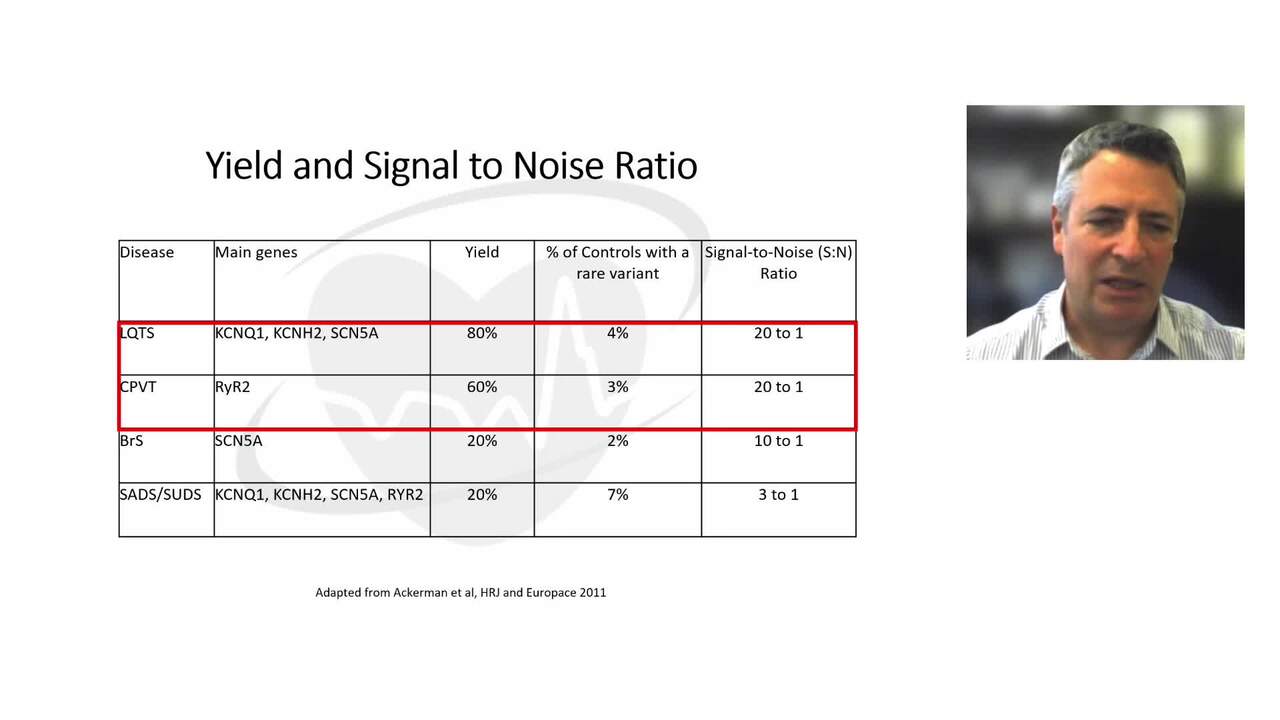
What is genetic variation and how does it cause cardiac disease?
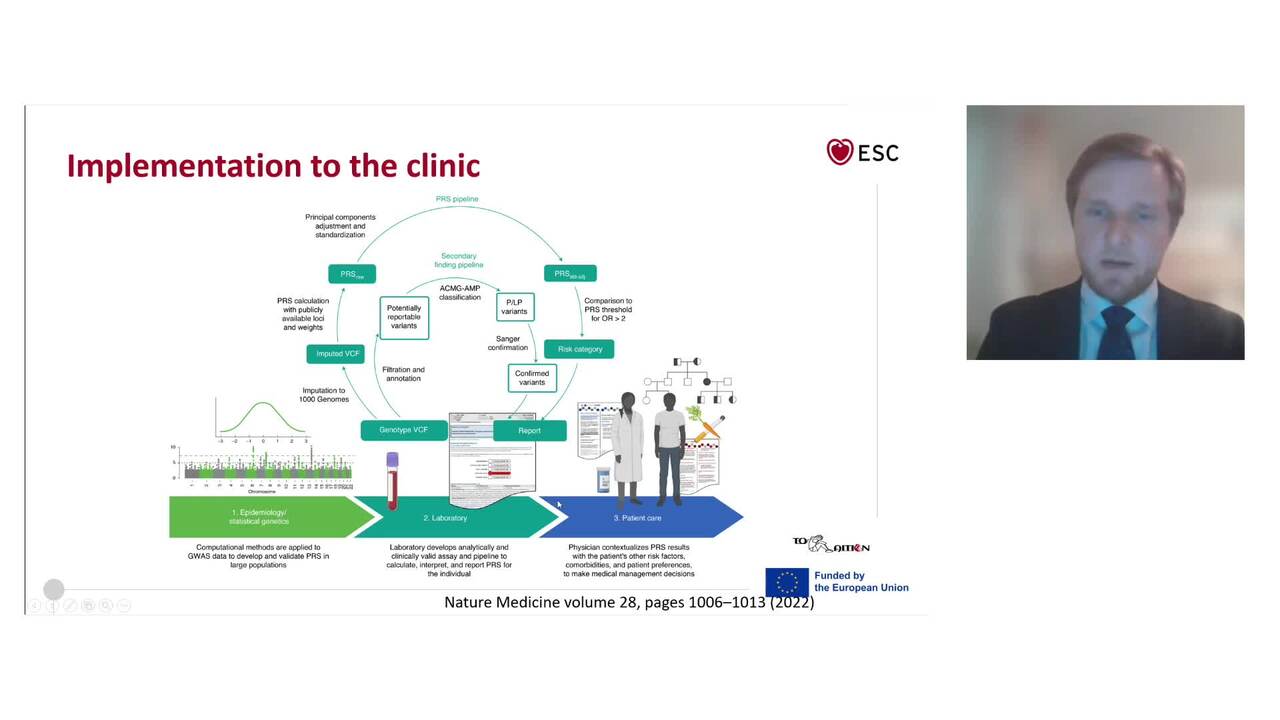
Genomics of cardiovascular risk factors
Test yourself - eLearning courses





















