Background
The definition of cardiovascular (CV) disease as a three stage continuum is well established, and has been for twenty years. The first stage of disease is when the CV risk factors are present. The existence of target organ damage (TOD), often represented in clinical practice by the appearance of chronic kidney disease (CKD) (albuminuria and/or an estimated glomerular filtration rate value-eGFR- below 60 ml/min/1.73 m2) or by the presence of EKG left ventricular hypertrophy (LVH), is regarded as the second stage. A superior level of atherosclerosis and a shorter time to the establishment of CV events is characteristic of this stage. The existence of CV events is considered the third and last stage of the CV continuum.
Hypertension is prevalent in the broad population: 44% in Europe when using 140/90mmHg as threshold. High blood pressure (BP) is defined as the most relevant CV risk factor due to its importance in the development and evolution of CV events. All guidelines identify the requirement of achieving a tight BP control (1,2), independently from the pharmacological drug family selected. Nevertheless, since the early 90s, the administration of angiotensin converting enzyme inhibitors (ACEis) have revealed properties that not only have led to the lowering of BP in a similar manner as other antihypertensive drugs, but also in the ability to protect the CV and renal systems (mainly in heart failure, post-myocardial infarction and in CKD - particularly diabetic nephropathy with proteinuria), in addition to the advantage reached by lowering BP. Similar positive effects were demonstrated later for angiotensin receptor blockers (ARBs).
The efficacy of ACEis and ARBs in the final stage of the CV continuum, jointly with their ability to prevent and regress TOD (above all albuminuria and LVH), has led to broad use of these drugs in the first stages of the continuum. Renin-angiotensin-aldosterone system (RAAS) suppression has also been the most common form of monotherapy in the hypertensive cohort of the last years.
However, all through chronic treatment with either ACEis or ARBs, angiotensin and aldosterone, a breakthrough appears to be the decrease in their ability to suppress RAAS. So much so that the benefits of diminishing the rate of evolution of CV disease is thereby restricted and, what has become demonstrable in recent years, is that cardiorenal disease development can be observed even with ongoing treatment of RAAS suppression (3).
Dual blockade : Utility in Clinical Practice.
The association of an ACEi and an ARB was originally considered as a means to achieving a powerful blockade of RAAS that would improve outcome further than from BP effects alone. Combined treatment with both has become (figure 1) an efficient therapeutic option in subjects with proteinuric nephropathies and congestive heart failure (CHF) and incomplete neurohormonal suppression (individuals without beta-blockers or intolerant to a sufficient dose of an ACEi) (4).
On the other hand, when compared to either of these drugs used in monotherapy, results from the "ONgoing Telmisartan Alone and in combination with Ramipril Global Endpoint Trial study" (ONTARGET)(5) have revealed that this kind of combination offers no benefit in patients with high global CV risk. This combination also shows an increase in the development of side effects, with the related exception of CHF and/or proteinuria. Moreover, BP control with this type of dual suppression, when compared to that reached by either ACEis or ARBs used in combination with a diuretic or a calcium channel blocker, has been widely described as minor (6).
Renin activity inhibition offers a therapeutic opportunity and has become helpful in limiting the first step of the RAAS cascade. Aliskiren is the first orally active direct renin inhibitor available. Used alone or in combination, in addition to leading to important BP reductions (7), has proved to be an active drug when administered on top of a sufficient dose of ARB to reduce albuminuria and LVH, as published in AVOID and ALLAY trials (8,9).
These recent results suggest that a combination of either an ACEis or an ARB with Aliskiren could improve the outcome of individuals with CV disease. Moreover, ongoing trials will offer the yet unknown data of its real potential in reducing CV events in high risk subjects.
The association of either an ACEi or ARB with an aldosterone receptor antagonist, both spironolactone and eplerenone, has been accepted as important complementary management of CHF. The Randomized Aldactone Evaluation Study (RALES) revealed that treatment with spironolactone largely decreased morbidity and mortality in patients with severe CHF (10). In the Eplerenone Post-acute myocardial infarction Heart Failure Efficacy and Survival Study (EPHESUS), eplerenone obtained a significant reduction in the morbidity and mortality associated with left ventricular dysfunction and CHF in the postmyocardial infarction patient when compared to placebo (11). Similar positive effects with spironolactone on top of both ACEis and ARBs for preventing the progression of chronic kidney disease (12) and in subjects with true resistant hypertension (13) have been published.
Figure 1. Effects of dual blockade with ACEi and ARB
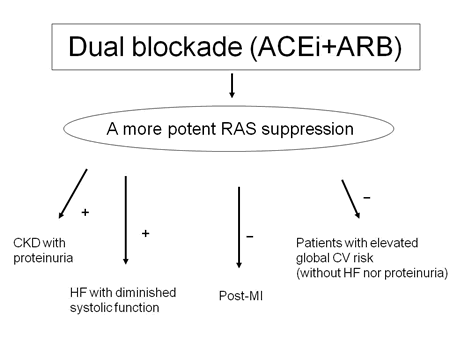
ACEi: Angiotensin converting enzyme inhibitor. ARB: Angiotensin receptor blocker. RAS: Renin-angiotensin system. CKD: Chronic kidney disease. HF: Heart failure. MI: Myocardial infarction. CV: Cardiovascular.
Conclusion:
RAAS suppression through either ACEis or ARBs in monotherapy has shown favourable CV effects, but it has several limitations. Dual blockade with aldosterone receptor antagonists offers positive outcomes in nephropathies and in CHF in a limited number of patients.
Future randomized trials with direct renin inhibitors and aldosterone receptor antagonists on top of both ACEis and ARBs will possibly show results that will help to support the benefits of dual blockade, through the obtaining of a decrease in CV events while maintaining an acceptable safety profile.


 Our mission: To reduce the burden of cardiovascular disease.
Our mission: To reduce the burden of cardiovascular disease.