1 - Resistant hypertension
The 2007 European Society of Hypertension/European Society of Cardiology Guidelines on Hypertension define “resistant hypertension” as the clinical condition in which blood pressure values are above 160/90 mmHg despite the use of at least 3 antihypertensive drugs (one of which being a diuretic) at full daily dosage. (1).
A similar definition has been used by the American Heart Association in a recent scientific statement (2).
Consensus regarding the definition of resistant hypertension, however, it does not apply to other aspects of the disease, such as epidemiological profile nor recommended therapeutic intervention. Epidemiological surveys estimate that 20%-30% of all hypertensive states may be resistant to treatment. Other investigations have provided, however, entirely different figures (from 7% to 13%), presumably due to the use of more stringent criteria for defining “resistant” - a given hypertensive state in which treatment fails to control blood pressure.
Indeed, a number of factors, such as the type of blood pressure measurement, the occurrence of a white coat phenomenon, poor adherence to treatment, the presence of an obese state or other drugs interfering with blood pressure control may be responsible for “pseudoresistance” and thus should not be included in the disease prevalence (2-3). Moreover, there are secondary causes of hypertension, such as obstructive sleep apnoea, renal parenchimal disease, primary aldosteronism and phoeochromocytoma that can be detected in patients with resistant hypertension and require to be excluded in the correct definition of the disease (2-3).
As emphasised in recent papers and official documents, the problem of resistant hypertension treatment still remains largely unaddressed (3-4). Among the recommended approaches, the use of mineralcorticoid receptor antagonists stands as the emerging one (2-3). It should be noted, however, that evens the anti-aldosterone drug approach encompasses not infrequent problems related to the patient’s adherence to treatment, due to the side-effects profile of the drug (5). Some favourable results might be obtained in the near future with endothelin-receptor antagonists, which however combine a proven efficacy to an unfavourable side-effects profile (fluid retention and oedema occurring in about ¼ of treated patients) (6).
2 - Renal denervation
The renal denervation approach is based on solid background related to the crucial role sympathetic renal nerves have in the development as well as in the progression of essential hypertension (Figure 1) (7). Preclinical experimental studies carried out in different animal models of hypertension have shown that the procedure may indeed decrease blood pressure values favourably thus interfering with cardiovascular homeostasis control (7). These promises have been confirmed in patients with resistant hypertension, in which a catheter-based renal denervation has been recently developed. In brief, the approach is based on the use of a catheter connected to a radiofrequency generator which is percutaneously positioned into the left and right renal artery. The radiofrequency-based ablation procedure lasts 2 minutes and is repeated 5 times at most in view of obtaining complete renal denervation. The first clinical experience with the device has been carried out in a group of 45 middle age patients with resistance hypertension and blood pressure values amounting to 177/101 mmHg (8). In the 12 month period following renal denervation there was a consistent and progressive blood pressure reduction that at the 1 year follow-up period amounted to 27/17 mmHg. The blood pressure reduction was by a significant decrease (amounting on average to about 50%) in systemic norepinephrine spillover, indicating the occurrence of sustained and generalised sympathoinhibition (8).
3 - Carotid baroreceptor stimulation
Carotid baroreceptors physiologically modulate autonomic tone, by inhibiting sympathetic cardiovascular drive and stimulating vagal influences on the heart (Figure 1). This homeostatic function is impaired in hypertension, leading to marked vasoconstriction and tachycardia. Preliminary studies in experimental animals have been conducted to try to restore the baroreceptor function. Results show that the procedure is able to lower blood pressure as well as reduce circulating levels of norepinephrine (9). Recently the implantation of a permanent bilateral perivascular carotid sinus pulse generator for carotid baroreceptor stimulation has been made feasible in patients with resistant hypertension. According to the results of a recently published paper (10), the stimulation procedure caused sustained blood pressure reduction (31/14 mmHg) coupled with consistent sympathoinhibition, without any major side effects.
4 - Unanswered questions
Although intriguing, the results of the two new approaches for the treatment of resistant hypertension leave room for a number of clinically relevant questions. First, are the favourable effects of the two interventions maintained over time? Second, does a reinnervation of the kidneys occur in the long-term? Is this process capable in some way to abolish the favourable effects of the procedure? Further, as far as carotid baroreceptor stimulation is concerned, is there any evidence of a time-dependent baroreflex desentisation to the electrical stimuli? What about the long-term safety of the procedure? Which are the effects of the two interventions on blood pressures alternative to the clinic one, i.e. ambulatory as well as home blood pressure?
Altogether these questions demonstrate that much needs to be learned about the two procedures, which nevertheless open new scenarios for the treatment of resistant hypertension.
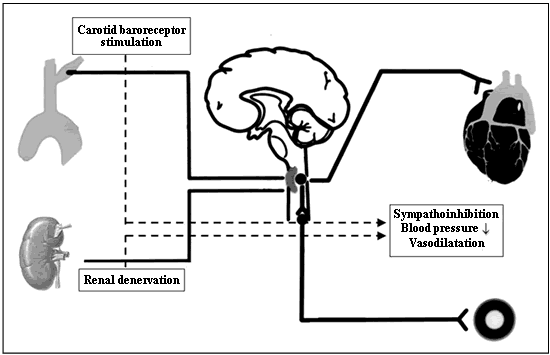
Fig1 : Strategies for treatment of Resistant Hypertension


 Our mission: To reduce the burden of cardiovascular disease.
Our mission: To reduce the burden of cardiovascular disease.