Background
Heart failure (HF) is a major public health issue and has become one of the most significant causes of morbidity and mortality for older adults in the U.S. and other Western countries.(1, 2) According to the American Heart Association (AHA), 550,000 new cases occur in the U.S. each year, and more than 5 million Americans have HF. Hospital discharges for HF have increased by 155% over the last 20 years, and HF is the most frequent cause of hospitalisation in persons aged 65 years or older (1). In Europe, 10 million people have HF according to the estimates of the European Society of Cardiology (ESC). The prevalence of symptomatic HF ranges between 0.4% to 2% in the general European population.(2)
I - All studies
There is ample evidence that regular physical activity has a protective effect against hypertension, coronary heart disease (CHD) and stroke (3). Regarding Heart Failure, here is the evidence we review :
a) Physical activity
Only two studies have assessed the association between physical activity and HF and results were inconsistent.
b) Leisure-time, physical activity and HF risk
In the First National Health and Nutrition Examination Survey, the significant inverse association between leisure-time, physical activity and HF risk was found only in women but not in men.
c) Vigorous physical activity
In a recent analysis from the Physicians’ Health Study, vigorous physical activity was associated with a decreased risk of HF (4)
d) Overweight
Evidence from epidemiological studies has shown that overweight (body mass index [BMI] 25-29.9 kg/m2) or obesity (BMI ≥30 kg/m2) is a major established risk factor for CHD and ischemic stroke(5). However, the results of the previous studies were contradictory as in some studies overweight (BMI 25-29.9) was found to be a strong risk factor for HF (5,9) but not in other studies (7, 8).
e) General obesity (BMI≥30)
Several studies have indicated that general obesity was associated with an increased risk of HF.4, (6-8).
f) Waist circumferance
It has been reported that greater abdominal (central) adiposity is associated with an increased risk of CHD, (5) however, only three recent prospective studies have assessed its possible effect with the risk of HF (9-11). A recent Swedish study indicated that a greater waist circumference was associated with HF at all levels of BMI in women, and both BMI and waist circumference were predictors among men (9).
In the Uppsala Longitudinal Study of Adult Men cohort, a 1-SD increase in waist circumference was associated with a 36% (95% CI 10%-69%) increased risk of HF.(10) The Multi-Ethnic Study of Atherosclerosis study found that abdominal obesity was associated with an increased risk of HF.(11). In the present study, we found that a greater waist circumference or waist-hip ratio was associated with a greater risk of HF in both men and women.(12)
g) Physical activity and BMI with HF risk
Until now, only the Physicians’ Health Study has evaluated the joint associations of physical activity and BMI with HF risk, and found that overweight and obesity was associated with a greater risk of HF and vigorous physical activity was associated with a reduced risk of HF. (4) BMI and vigorous physical activity did not modify one another’s individual effect on HF risk. Lean and active individuals had the lowest risk of HF, while obese and inactive individuals had the highest risk. (4) However, this study used self-reported height and weight and had no data on waist and hip circumference.
II - The Finnish FINMONICA study
Single and joint associations of physical activity and different indicators of adiposity with HF risk.
The Finnish FINMONICA study also evaluated the single and joint associations of physical activity and different indicators of adiposity - BMI, waist circumference, and waist-hip ratio). (12). Study cohorts comprised 59,178 Finnish participants who were 25 to 74 years of age and free of HF at baseline. During a mean follow-up of 18.4 years 1921 men and 1693 women developed HF.
1 - Low, moderate and high physical activity
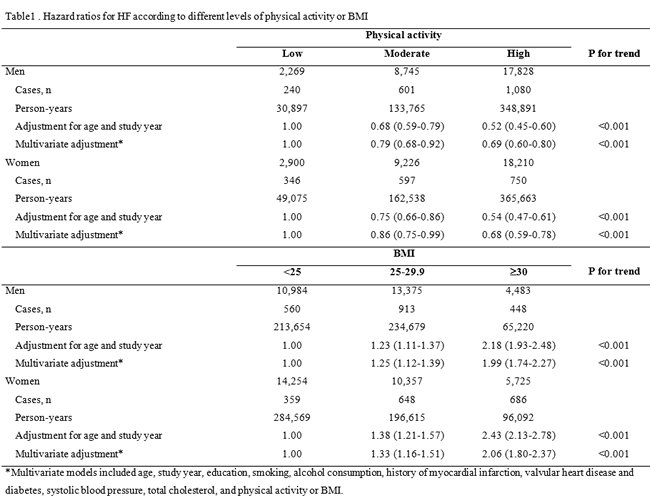
The multivariable-adjusted (age, study year, smoking, education, alcohol consumption, history of myocardial infarction, history of valvular heart disease, BMI, systolic blood pressure, total cholesterol, and history of diabetes) hazard ratios (HRs) of HF associated with low, moderate and high physical activity were 1.00, 0.79, and 0.69 (Ptrend<0.001) for men, and 1.00, 0.86, and 0.68 (Ptrend<0.001) for women, respectively (Table 1).
2 - Different levels of BMI
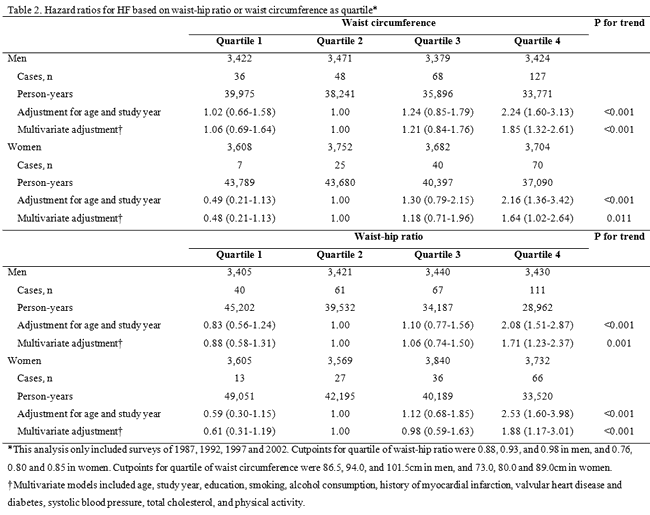
The multivariable-adjusted HRs of HF at different levels of BMI (<25, 25-29.9, and ≥30) were 1.00, 1.25, and 1.99 (Ptrend<0.001) for men, and 1.00, 1.33, and 2.06 (Ptrend<0.001) for women, respectively (Table 1). The multivariable-adjusted HRs of HF across quartiles of waist circumference (quartile 2 as the reference group) were 1.06, 1.00, 1.21, and 1.85 (Ptrend<0.001) in men, and 0.48, 1.00, 1.18, and 1.64 (Ptrend=0.011) in women, respectively (Table 2).
3 - Waist-hip ratio
Similarly, the multivariable-adjusted HRs of HF across quartiles of waist-hip ratio were 0.88, 1.00, 1.06, and 1.71 (Ptrend<0.001) in men, and 0.61, 1.00, 0.98, and 1.88 (Ptrend<0.001) in women, respectively (Table 2).
4 - Physical activity and BMI
In joint analyses of physical activity and BMI on HF risk, the protective effect of physical activity was consistent in subjects with any levels of BMI (all Ptrend<0.05).
5 - Physical activity and waist circumference or waist-hip ratio
The joint associations of physical activity and waist circumference or waist-hip ratio with the risk of HF were inconsistent.
- The protective effect of physical activity was found in subjects with low waist circumference (Ptrend<0.01) and subjects with high waist-hip circumference(Ptrend<0.01).
- The positive association of waist-hip ratio with HF risk was consistent in subjects at all levels of physical activity (all P<0.001), however, the positive association of waist circumference with HF risk was only found in subjects with moderate (P<0.001) or high level of physical activity (P<0.01).
Conclusion:
The results from our study shows that subjects with general overweight and general and abdominal obesity are independently associated with an increased risk of HF, while physical activity is associated with a reduced risk of HF among both men and women. The protective effect of physical activity on HF risk is observed at all levels of BMI.


 Our mission: To reduce the burden of cardiovascular disease.
Our mission: To reduce the burden of cardiovascular disease.