For many years, hypertension has been recognised as a major risk factor in the development of cardiovascular diseases. One of the main problems in hypertension is its definition. Many mistakes are made at the time of blood pressure measurements and these mistakes can have far reaching consequences.
They may be generated from using a faulty manometer, a non adapted cuff, from stenosis at the level of the brachial artery or, as it is most often the case, from misinterpretation of the readings by the physician.
Also, one must realise that blood pressure is not a constant value. Blood pressure varies from one moment to the next, day readings are different from night readings etc. These variations are largely due to the conditions encountered in real life and also depend on the circumstances at the time of blood measurements themselves (whether at the doctor’s office, at home or at work …).
Consequently, blood pressure measurements should no longer be seen as a set of numbers, but rather, as forming a curve that is permanently “floating” over 24 hours and is influenced by all factors acting on the cardiovascular system.
Thus, to define someone’s “real” blood pressure, one should overcome all technical problems but also provide the observer with information on the variations of blood pressure over a certain period of time (for ex. 24 hours).
In the last thirty years, several techniques have been developed to try to achieve this. First intra-arterial recordings were made on an ambulatory basis. Because of the risk linked to this technique, non-invasive techniques were set up to enable the recording of blood pressure in normal life conditions over 24 hours and even longer. The definition of blood pressure is reached by recording either the Korotkoff sounds or the oscillations at the level of the brachial artery. Inflation and deflation of the cuff is fully automated and data are stored in a memory chip placed inside a portable recorder. Results must then be checked and fully validated according to international guidelines.(1).
An example of such 24 hour ambulatory recordings is given in fig.1. You may clearly see that blood pressure rapidly increases in the early morning, decreases in the afternoon and increases again at the end of the afternoon and evening, and dips during the night. Recording 24 hour ambulatory blood pressure fully illustrates the large variations of blood pressure; it can easily be understood that there are large differences when compared to data collected from the few readings at the doctor’s office.
The real question that follows such an observation is: what are the blood pressure readings that really matter for the patient? Which pressure determines long term prognosis and with what pressure to proceed in the clinic to define and follow up someone’s overall blood pressure.
Many aspects of this question have been answered in a recent study which compares over a long term, office pressure and 24-hour ambulatory pressure in treated hypertensive patients (the Office versus Ambulatory blood pressure study, OvA) (2).
A group of 1963 patients with mild to moderate hypertension were followed over a period of at least five years, yielding approximately 10.000 patient/years; all events were carefully recorded, analysed and reviewed by an expert committee. All patients were treated according to international guidelines; the choice of antihypertensive drugs was left to the discretion of the physician. At yearly intervals, all data obtained were reviewed and control examinations were made on office and ambulatory blood pressure. Close attention was given to obtain, through treatment, an office blood pressure control down to 140/90 mm Hg. To determine whether office or ambulatory pressure is best to predict events, correlations were calculated between events and office pressure on one hand and between events and ambulatory pressure on the other hand.
Quite clearly, all blood pressure figures, including the simple office readings, correlate with long term prognosis. This is a confirmation of many previous studies and makes clear that whatever the type of blood pressure measurement, the level of blood pressure is related, step by step, to long term prognosis. However, when office and ambulatory blood pressure are compared vis-a-vis their relation to long term prognosis, it comes out that ambulatory blood pressure predicts prognosis much better than (“over and above”) office pressure. This also holds true after an adjustment is made from all existing risk factors.
Besides this main message, many other pieces of information came out of this study. Systolic blood pressure does clearly better in predicting prognosis than diastolic blood pressure. This also holds true in several recent studies amplifying the importance of systolic blood pressure elevation (3) One should not, nevertheless, deny the role of diastolic blood pressure.
Lastly, elements of information are yielded in a new class of patients - i.e. in those whose office pressure is lower than ambulatory pressure-; this new entity is often called “reversed” or “masked” hypertension.
The clinical value of reversed hypertension was clearly illustrated in this study as shown by the following finding: prognosis of patients with high office pressure but with low ambulatory pressure is better than prognosis of patients with low office but with high ambulatory pressure.
One must realise the clinical repercussions of this finding: the first situation is regularly quoted as bad blood pressure control since office readings are above the goal values described in the guidelines; the second situation is precisely the opposite as it shows good control of office pressure. Yet, prognosis is worse in the latter situation.
Several conclusions can be drawn from this study. First, it confirms previous studies that have shown that, in a vertical relation, ambulatory blood pressure correlates better than office readings with parameters of organ damage such as left ventricular hypertrophy (4). But the present study goes far beyond this statement yet as it clearly shows that this better correlation also has long term repercussions and ambulatory blood pressure recordings predict cardiovascular morbidity and mortality significantly better than office readings.
Second, this leads to a revision in the indications for ambulatory blood pressure recordings. Up to now, it was stated that ambulatory recordings should be made whenever there is a contradiction between office readings and clinical symptoms or parameters of organ damage (for example high office values and no left ventricular hypertrophy), in patients with so-called resistant hypertension (many of them have much lower ambulatory readings that can be predicted from office readings), patients showing many side effects on even low doses of antihypertensives (as their blood pressure often is very much lower than anticipated) and of course, in research conditions.
However the present data give a much broader scope for ambulatory blood pressure recordings. There is a clear argument that such recordings should be made in all hypertensive patients on treatment whatever their achieved office blood pressure is. Such recordings should be repeated at regular intervals.
In all, one can hope that the implementation of these conclusions should be made possible by making the technique easier and cheaper. Social security and/or insurance systems should work at a proper reimbursement of the technique. Also there could come an appealing association with home blood pressure recordings that could provide a filter to define in which patients ambulatory pressure should be recorded soas to yield optimal clinically useful information (5).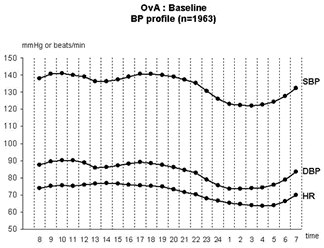
Fig.1. Means of twenty-four hours blood pressure profiles of all patients included in the OvA study.
(SBP: systolic blood pressure; DBP: diastolic blood pressure; HR: Heart rate).
The content of this article reflects the personal opinion of the author/s and is not necessarily the official position of the European Society of Cardiology.


 Our mission: To reduce the burden of cardiovascular disease.
Our mission: To reduce the burden of cardiovascular disease.