Introduction
Atrial fibrillation (AF) is the most frequent arrhythmia with increasing incidence in concordance with aging, reaching up to 10% prevalence in the population over 75 years [1].
Alongside the accumulation of different cardiovascular diseases and risk factors, aging itself is a condition predisposing to AF, characterised by myocardial fibrosis and atrial dilatation. Human aging produces changes in electrophysiological and electro-anatomical characteristics of the atrial myocardium.
Although AF itself cannot be considered as a cause of death, the presence of AF doubles all-cause mortality due to sudden death, heart failure or stroke [2].
In addition to appropriate anticoagulation for stroke prevention (as a cornerstone in the therapy for AF), rate and rhythm control are two of the main long-term therapeutic strategies [3]. As in other areas of medicine, age is no longer a limiting factor to different modalities of treatment which include all kinds of invasive techniques.
However, it should be borne in mind that the objectives of treatment are to be met for a number of years, not decades. The level of activity in the elderly is not the same as it is in young people; medication tolerance can be lower and the number of comorbidities is higher.
Rate control therapy in atrial fibrillation
Rate control is the first-line therapy in elderly patients. Usually, this is sufficient to control the symptoms in symptomatic patients and it is also the treatment choice in asymptomatic patients. Rate control allows AF to persist, controlling the heart rate with medications that slow down the conduction through the atrioventricular (AV) node.
The evidence concerning which is the best type of rate control and its intensity level is unclear.
Acute rate control
Acute rate control refers to an acute slowing of the heart rate where haemodynamic stability is achieved. The underlying causes of a high heart rate in new-onset AF could be acute infection, anaemia, endocrine imbalance, pulmonary thromboembolism, etc. If high sympathetic tone is suspected as a reason for the high heart rate, then beta-blockers or non-dihydropyridine calcium channel blockers (CCB) are preferred over digoxin.
If the patient has a left ventricular ejection fraction (LVEF) <40%, then beta-blockers and/or digitalis are preferred over CCB, because CCB have negative inotropic effects [4].
In critically ill patients and those with severely impaired LV systolic function, intravenous amiodarone can be used where excess heart rate is leading to haemodynamic instability [3]. Urgent cardioversion should be considered in haemodynamically compromised patients [3].
Long-term rate control
Long-term rate control can be achieved by applying monotherapy or a combination therapy of beta-blockers, digoxin and non-dihydropyridine CCB. The choice is often made on an individual basis after scanning the patient’s characteristics and comorbidities.
Although the prognostic benefit of beta-blockers seen in heart failure with reduced ejection fraction (HFrEF) patients and sinus rhythm is lost in patients with AF [5], beta-blockers are still first-line rate control agents [3]. This recommendation is based on the potential of beta-blockers to improve symptomatic and functional status, the lack of harm in any AF patient and the good tolerability profile across all ages [6].
Non-dihydropyridine CCB can be used as an alternative, due to the fact that they provide reasonable rate control and improve symptoms; however, they should be avoided in heart failure (HF) patients because of their negative inotropic effect [4].
Comparative drug trials of beta-blockers versus non-dihydropyridine CCB have not shown advantages of one agent over another. The data from post hoc analysis of the AFFIRM trial [6] showed that patients initially treated with beta-blockers were less likely to change their medication in comparison with those initially treated with CCB. There is no evidence that better rate control can be achieved with any of these medications. It is reasonable to switch from one medication to another in patients who have an inadequate response to the initial treatment.
Cardiac glycosides, such as digoxin and digitoxin, are medications of choice in HF patients [6]. On the other hand, digoxin has been proven to be an independent risk factor for death in patients without HF and should be used cautiously in the elderly, especially those with impaired renal function [7]. All studies showing an excess mortality rate with digoxin are observational. Given the lack of a randomised trial, we could also suspect prescription bias, because digoxin was usually prescribed to sicker patients.
The question as to whether digoxin is safe enough to be used routinely in AF patients remains open. There are more data which show that mortality rate depends on serum concentrations of digoxin [8]. However, lower doses of digoxin (≤250 mg once daily), corresponding to serum digoxin levels of 0.5-0.9 ng/mL, may be associated with a better prognosis [3].
Amiodarone is the drug of choice for rate control, yet it has considerable extracardiac adverse effects. According to the ESC Guidelines, it should be used as a last resort drug in patients whose heart rate cannot be controlled with combination therapy [3].
Membrane active rhythm control medications, such as flecainide or sotalol, are not recommended for rate control, because the potential pro-arrhythmic effect outweighs the usefulness of rate control.
Rate control is also a choice of treatment in patients where rhythm control was not successful. It is important that rate control AF patients are kept under regular and close surveillance for the potential development of tachycardia-related cardiomyopathy. In case of symptoms or signs of left ventricular dysfunction, we should consider a change of treatment strategy (rhythm control or ablate and pace strategy).
Strict versus lenient rate control
The optimal heart rate target in AF patients is undetermined. The first randomised trial addressing this issue, RACE II, compared two target heart rates: a) 80 bpm at rest, 110 bpm during moderate exercise (strict heart rate), and b) 110 bpm at rest (lenient heart rate). A difference in composite clinical events, NYHA class or hospitalisations was not found [9]. Strict rate control also does not seem to affect the mortality rate [9]. Cardiac remodelling (left atrial and left ventricular size) did not occur to a greater extent in the group with lenient rate control. No benefit concerning symptoms and quality of life was shown with a strict rate control. At the end of follow-up, the mean resting rate in the lenient rate control group was 85 bpm, versus 75 bpm in the strict rate control group [9].
The findings of this study suggest that lenient rate control may be an acceptable strategy, for as long as patients remain asymptomatic or minimally symptomatic. In addition, it is convenient because it requires fewer outpatient controls and less monitoring.
To conclude, whether a strict or lenient rate control strategy should be followed is entirely up to the responsible doctor, bearing in mind the symptoms, avoiding bradycardia on the one hand and avoiding development of tachycardia-mediated cardiomyopathy on the other.
Rhythm control therapy in atrial fibrillation
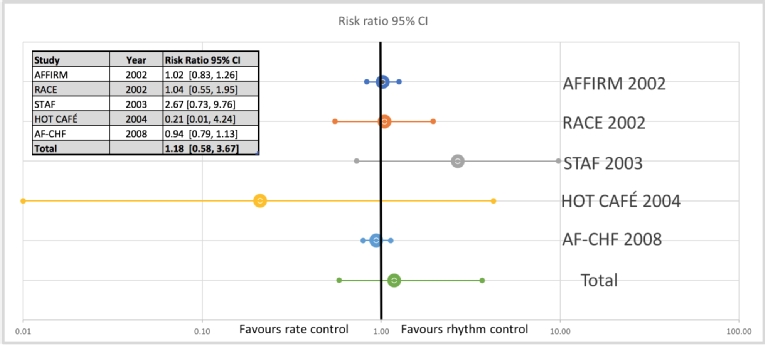
Rhythm control consists of cardioversion to normal sinus rhythm, usually followed by medications for sinus rhythm maintenance or non-pharmacologic rhythm treatment (e.g., catheter ablation). In spite of a natural tendency to believe that maintaining sinus rhythm brings better prognoses in AF patients, many of the trials conducted comparing rhythm and rate control strategy showed no difference in stroke risk, morbidity and mortality (Figure 1).
Figure 1. Forest plot for cardiovascular mortality.
AFFIRM: Atrial Fibrillation Follow-up investigation of Rhythm Management study; RACE: Rate Control versus Electrical Cardioversion for Persistent Atrial Fibrillation study; STAF: Strategies of Treatment of Atrial Fibrillation study; HOT-CAFÉ: How to treat Chronic Atrial Fibrillation study; AF-CHF: Atrial Fibrillation and Congestive Heart Failure study; CI: confidence interval
Pharmacological cardioversion is successful in approximately half of the patients with AF [3], usually in patients with recent onset of AF. It is convenient for older patients because it does not require sedation. Amiodarone can be used for pharmacological cardioversion safely and effectively in all patients [3]. In the absence of structural heart disease, IV flecainide, propafenone or vernakalant could be the treatment of choice. A “pill in the pocket” strategy with flecainide and propafenone may also be recommended [3].
Electrical cardioversion is mandatory in haemodynamically compromised patients [3]. It is a treatment of choice if the ventricular rate is fast, without immediate response to IV medications, or followed by myocardial ischaemia, hypotension or HF. Electrical cardioversion should be avoided if AF episodes are very frequent and repeating and in case of digitalis intoxication or hypopotassaemia [10].
Electrical cardioversion can be performed safely in older patients, under sedation and continuous monitoring of blood pressure and oximetry. Available temporary pacing is mandatory to avoid unnecessary bradycardia episodes.
After successful pharmacological or electrical cardioversion, medications are usually given to maintain a sinus rhythm. For maintenance of sinus rhythm, especially in the older population, the choice of drug should be guided by its safety profile, and coexisting heart, renal or hepatic diseases.
Amiodarone as a long-term therapy choice has many extracardiac side effects and should not be a first-line treatment choice, although it is most effective and safe in patients with HF [3]. To avoid pro-arrhythmic effects, the QT interval should be monitored on a regular basis.
Administration of Class I antiarrhythmic drugs in elderly patients should be very cautious, bearing in mind that these drugs are reserved for patients without structural heart disease. Close monitoring of the QRS duration is recommended, and widening of more than 150% of the baseline QRS should lead to dose reduction or treatment withdrawal [3].
A general AF guideline recommendation is to limit the use of quinidine, dysopyramide, dofetilide and sotalol to specific situations. This is even more true for the elderly. Long-term rhythm control therapy should be reserved for symptomatic patients with AF. There is no evidence to support sinus rhythm maintenance in asymptomatic patients at the cost of exposing them to the serious side effects of antiarrhythmic drugs. ECG monitoring serves as a tool for risk assessment. After the onset of antiarrhythmic drug treatment, one should monitor the duration of the PR interval, QRS and QT interval.
The use of beta-blockers for maintaining sinus rhythm is very safe, but not effective enough. Small trials have found a lower risk of AF recurrence after cardioversion in patients treated with sustained release metoprolol [11].
The decision to follow the rhythm control strategy, especially in the elderly, should be fully discussed between the responsible doctor and the patient.
Antiarrhythmic drugs in elderly patients
Older patients usually have coexisting heart, renal, or hepatic diseases, which can cause limitations of treatment with antiarrhythmic drugs.
Beta-blockers are probably the most used, investigated and safe medications in this age group. However, there are some differences between different beta-blockers. For example, carvedilol is a less potent beta-adrenergic blocker compared to others. Metoprolol succinate and bisoprolol have the advantage of single daily dosing; both are safe in HF patients.
Being of low lipophilicity, atenolol and nadolol have the advantage of fewer central nervous system side effects when compared to other beta-blockers. However, they are not appropriate for HF patients and should be avoided in patients with renal dysfunction. Adverse effects of beta-blockers include extreme slowing of AV conduction, hypotension, reduced exercise tolerance or acute worsening of HF.
Verapamil and diltiazem are negative inotropic agents and should be avoided in HF patients. A combination of these agents with beta-blockers could produce severe bradycardia or severe prolongation of AV conduction including different degrees of AV block. Caution should be exercised if digoxin is included in concomitant therapy, because verapamil increases serum levels of digoxin.
As mentioned before, increased serum levels of digoxin are associated with an increased mortality rate [7,8]. Digoxin is not recommended as a first-line therapy or monotherapy, because it affects only the resting ventricular rate and has no effect on the ventricular rate during effort. Older patients who are not physically active or who are disabled may still benefit from digoxin therapy. However, in acute HF and with a rapid ventricular rate, digoxin is the only drug of choice because beta-blockers and CCB are contraindicated. In HF patients who cannot tolerate higher doses of beta-blockers, low doses of digoxin can be added to reach the desired heart rate and symptom control. When digoxin is used, serum concentration should be monitored, with the goal of maintaining levels <1.2 ng/mL [8].
Due to its long-term side effects, oral amiodarone as a rate control agent is avoided in younger patients but should be considered in the elderly, especially if they are refractory to other medications. It has less frequent side effects in terms of pro-arrhythmia, bradycardia or hypotension.
Membrane active antiarrhythmic agents have been associated with induction of proarrhythmia. In conditions of impaired function of the liver and kidneys, as can be expected in the elderly, side effects could be more pronounced. Evidence from different studies indicate that quinidine, flecainide, sotalol and dofetilide are the antiarrhythmics most prone to inducing ventricular proarrhythmia [12].
All Class I antiarrhythmic drugs are generally not recommended in the elderly. If indicated, administration of these drugs must be performed cautiously. PR, QRS, and QT duration should be closely monitored [3].
Dronedarone is another medication that should be given cautiously in the elderly. The PALLAS study showed that dronedarone is related to an increased risk of cardiovascular events in patients older than 75 years with hypertension and diabetes [13].
Catheter ablation of AF in the elderly
For years, patients over 75 years were excluded from catheter ablation trials for safety reasons. Improvements in ablation techniques have given elderly patients a chance for rhythm control treatment with a rate of complications comparable to a younger population.
In a large worldwide survey, major periprocedural and post-procedural complications of catheter ablation, including death, cardiac tamponade, strokes, and transient ischaemic attacks, were reported in 4.5% of cases, regardless of age at the time of the procedure [14].
Data from small retrospective studies show that the multiple procedure success rate for paroxysmal AF in patients over 75 years is comparable with younger patient cohorts; however, it was less favourable for persistent and long-standing persistent AF [15]. The safety profile was comparable with younger patient cohorts, with a major complication rate of 5.8% [15]. The study by Nademanee et al showed that elderly patients with AF benefit from AF ablation, which is safe and effective in maintaining sinus rhythm [16]. The complication rate during the first 24 hrs was 7.3%, out of which only 3.4% were major complications [16]. Only 6.5% of patients were re-hospitalised in the first month, 2.7% due to groin complications - bleeding, pseudoaneurysm - and 2.7% due to atrial tachycardia. Maintaining sinus rhythm in this population (aged over 75) by catheter ablation was feasible in approximately 80% of patients, although a significant number of patients required more than one procedure (44% of successfully ablated patients).
Cryoballoon pulmonary vein isolation seems to be a promising technique in elderly patients. The advantage over radiofrequency ablation is the lower risk of complications such as pulmonary stenosis or oesophageal injury. Small studies conducted in the elderly (over 70 years) show a very low rate of minor complications, e.g., transient phrenic nerve palsy or groin haematoma [17].
If sinus rhythm maintenance is not achieved by an ablation procedure, sometimes only symptom relief in patients with drug-resistant AF might be considered as a positive outcome even if drug therapy is not discontinued.
Rate or rhythm control in heart failure patients
HF and AF are conditions in older patients that often coexist and promote each other. The danger of proarrhythmia and the negative inotropic effect of many antiarrhythmic drugs are limiting factors for their use in HF patients. However, maintenance of sinus rhythm is possibly most important in this subgroup of patients, due to the positive effect of sinus rhythm on functional status and the possible reduction in mortality [18]. As such, ablation has been proposed as a more efficacious way of achieving sinus rhythm. Most of the positive results of ablation in HF patients stem from the CASTLE-AF study [18]. Ablation resulted in a lower AF burden (follow-up with ICD interrogation) and improved ejection fraction in the ablation group. However, these data cannot simply be transferred to elderly patients, given that the average age of patients in the CASTLE-AF study was 64 years. Subgroup analyses suggested that patients with advanced HF (Class 3 or 4) did not benefit from an ablation procedure. This study contributed to the definition of “successful ablation” as lowering AF burden instead of prevention of AF recurrence [18].
Ablate and pace strategy
There are a few small randomised clinical trials comparing pharmacological rate control and permanent pacing with complete AV node catheter ablation in patients with HF. These trials showed a benefit of an “ablate and pace” strategy in terms of symptom relief, HF hospitalisations and mortality [19]. AV node ablation solves the problem of rapid ventricular response in AF, which aggravates symptoms and HF.
Catheter ablation of the AV node and permanent pacing should be considered if pharmacological rate control fails [3]. The optimal choice of pacemaker type or pacing mode is still unclear.
Right ventricular or biventricular pacing is the next question which should be answered in the future. There are limited data suggesting an advantage of biventricular pacing versus right ventricular pacing in HF patients.
Rate or rhythm control – how to choose
A systematic review and meta-analysis of randomised controlled trials showed no significant differences in any outcome - all-cause mortality, cardiovascular mortality, arrhythmic/sudden death, ischaemic stroke, systemic embolism and major bleeding [20].
Table 1. Rate or rhythm control preferences.
| In favour of rate control | In favour of rhythm control |
|---|---|
| Asymptomatic patients | Symptomatic patients |
|
Successful rate control with medication (lenient rate control in asymptomatic patients) |
Unsuccessful rate control with medication |
| Patients with comorbidities | No comorbidities |
| Patients with heart failure class 3-4* | Patients with heart failure class 1-2* |
* No firm data available for patients over 75 years.
In the absence of clear data for rate or rhythm control preference in terms of life longevity, it is up to the responsible doctor or cardiologist to decide which strategy to follow. In this context, an individual approach to the patient and shared decision making are crucial. The patient and/or the family should be informed about the treatment possibilities in a clear and open conversation and a decision should be made with respect to the preference of the patient. One must bear in mind that an ablation procedure is an extensive procedure and expectations are usually more than palliation. Comorbidities and drug tolerance are other issues that should be considered when choosing a rate or rhythm approach for these patients.
Aggressive risk factor reduction
It has been shown that weight loss and risk factor management are an essential component in the treatment of patients with AF. The REVERSE-AF study looked at the association of weight loss and the natural progression of AF [21]. The 310% weight loss with management of other cardiovascular risk factors was associated with significant reversal of AF burden and reduction in the need for AF ablation [21]. These results are quite encouraging in terms of prevention of disease progression.
Risk factor management, including obesity treatment, should be part of the integrated care which the AF patient deserves.
Conclusions
The published data support the use of all available rate or rhythm control interventions, including pacemakers and transcatheter ablations, without any age limits. It is of the utmost importance to know that there are no data showing any increased harm from AF ablation in the elderly. Explanation to the patient should be very informative in terms of expectations of the ablation procedure. Ablation may not eliminate AF, but it can substantially reduce it, and there are no data for this age group confirming better outcome. Impaired renal or hepatic function must be considered if any drug treatment is recommended.
Usually the expectations of the elderly are focused on quality of life, symptom relief and the capability of coping with usual everyday activities. It is always helpful to know the patient's activity level, mental alertness and living situation. Bearing all that in mind, it is important to make a considerable effort to inform the patient and/or the family and to make joint decisions.