Hot Lines: Targeting iron deficiency in heart failure
27 Aug 2023
Previous studies have shown that ferric carboxymaltose (FCM) improves symptoms, quality of life and exercise capacity in patients with heart failure with reduced ejection fraction (HFrEF) and iron deficiency;1,2 however, further evidence is needed regarding its effects on clinical events.
 Hotline-Mentz.jpg
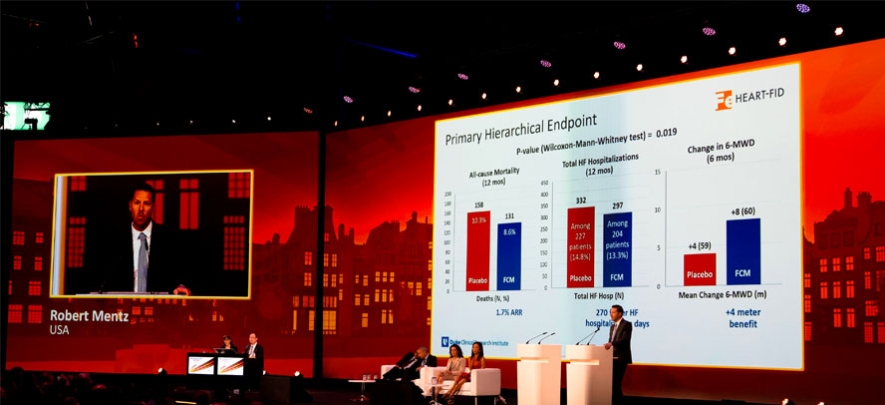
Hotline-Mentz.jpg In yesterday’s HF-themed Hot Line session, Doctor Robert Mentz (Duke University Medical Center - Durham, USA) presented results from the international HEART-FID trial. Participants had HFrEF (LVEF ≤40% within 24 months or ≤30% within 36 months), iron deficiency (haemoglobin >9.0 g/dL and <13.5 g/dL [females] or >9.0 g/dL and <15.0 g/dL [males], and ferritin <100 ng/mL or ferritin 100-300 ng/mL with a transferrin saturation [TSAT] <20%) and were on maximally tolerated background therapy for ≥2 weeks. In total, 3,065 patients were randomised to IV FCM or placebo, with doses administered at 0 and 7 days, and then every 6 months based on iron indices and haemoglobin levels. The average age was 69 years and 34% were women.
FCM resulted in modest numerical differences compared with placebo for each of the components of the hierarchical primary composite of all-cause mortality at 12 months, HF hospitalisations at 12 months and 6-month change in 6-minute walk distance (6MWD). Specifically, 8.6% of patients on FCM and 10.3% of patients on placebo died over the 12-month period, and there were 297 and 332 HF hospitalisations, respectively. The mean change in 6MWD at 6 months was 8 ± 60 m with FCM and 4 ± 59 m with placebo.
The unmatched win ratio for the overall composite was 1.10 (99% CI 0.99 to 1.23; p=0.019) and while this indicated 10% more wins with FCM, it did not meet the prespecified significance level of p=0.01.
For the top secondary endpoint of time to first HF hospitalisation or CV death, there were fewer events in the FCM group than placebo (16.0 versus 17.3 events per 100 patient-years; hazard ratio [HR] 0.93; 96% CI 0.81 to 1.06). The HR for the secondary endpoint of CV death was 0.86 (96% CI 0.72 to 1.03).
Dr. Mentz concludes, “The HEART-FID trial confirmed the safety of IV FCM in patients with HFrEF and despite suggesting potential outcome benefits, it did not meet its primary efficacy endpoint.”
Professor Piotr Ponikowski (Wroclaw Medical University - Wroclaw, Poland) then presented a meta-analysis of pooled individual participant data from 4,501 adult patients with HF and iron deficiency enrolled in HEART-FID and two other placebo-controlled trials investigating FCM, namely CONFIRM-HF and AFFIRM-AHF.
Over 12 months’ follow-up, FCM therapy significantly reduced the first co-primary composite endpoint of total CV hospitalisations and CV death compared with placebo, with a rate ratio (RR) of 0.86 (95% CI 0.75 to 0.98; p=0.029). There was a trend towards reduction of the second co-primary composite endpoint of total HF hospitalisations and CV death, but it failed to reach statistical significance (RR 0.87; 95% CI 0.75 to 1.01; p=0.076). FCM therapy was associated with a 17% relative rate reduction in total CV hospitalisations (RR 0.83; 95% CI 0.73 to 0.96; p=0.009) and a 16% relative rate reduction in total HF hospitalisations (RR 0.84; 95% CI 0.71 to 0.98; p=0.025). There was no effect of FCM administration on mortality.
In subgroup analyses, patients in the lowest TSAT tertile (<15%) derived greater benefit from FCM on the first co-primary composite endpoint than those with higher baseline TSAT (interaction p=0.019).
Summing up, Prof. Ponikowski comments, “These findings indicate that IV FCM should be considered in iron-deficient patients with HF and reduced or mildly reduced ejection fraction to reduce the risk of hospitalisation due to HF and CV causes.”
References
- Anker SD, et al. N Engl J Med. 2009;361:2436–2448.
- Ponikowski P, et al. Eur Heart J. 2015;36:657–668.


