Adverse cardiovascular effects of smoking
Cigarette smoking adversely affects the cardiovascular system via several mechanisms: hydrocarbons in smoke injure the arterial endothelium, promote low-grade inflammation and increase plasma fibrinogen, stimulate platelet aggregation and accelerate atherosclerosis; nicotine is associated with catecholamine release, which increases heart rate, raises arterial blood pressure, causes vasoconstriction and predisposes to cardiac arrhythmias; smoking also increases the level of carbon monoxide in blood which reduces myocardial oxygen delivery (1, 2). Smoking is strongly linked to peripheral arterial disease, myocardial infarction and sudden cardiac death (2).
Smoking status and early survival in acute myocardial infarction
During the past 20 years it has been consistently reported that smokers who suffer acute myocardial infarction (AMI) have a more favorable short-term prognosis than non-smokers. In the “thrombolytic treatment era” it had been postulated that the better response to thrombolysis in smokers was due to the more frequent thrombotic nature of coronary artery occlusion, presumably caused by a smoking-related hypercoagulable state, in contrast with the often more critical residual coronary stenoses found in non-smokers (1, 3). The crude in-hospital mortality of AMI treated with thrombolysis ranged from 2.3 – 4.7 % in smokers, to 5.2 – 7.6 % in former smokers, and to 7.0 – 13.8 % in non-smokers (1, 3-5).
In the “percutaneous coronary intervention treatment era” smokers with AMI have seemingly retained their survival advantage over former smokers and non-smokers with crude 30-day mortality rates of 1.3 % vs. 1.7 % vs. 3.5 % (6). However, after multivariate correction for differences in baseline variables smoking status was no longer protective from mortality: smokers were more than 10 years younger than non-smokers and had significantly lower rates of several factors that negatively affect prognosis – such as diabetes, hypertension, triple-vessel disease, left anterior descending coronary artery involvement, and being female (6).
It is noteworthy that the procedural success rates of percutaneous coronary intervention were similar in all groups in contrast to thrombolytic studies showing greater recanalization rates in smokers, attributed to the greater thrombus burden (6).
Baseline differences between smokers and nonsmokers with AMI
Already 20 years ago, a careful study of 2955 patients with AMI called attention to the fact that smokers were about a decade younger than non-smokers, had a lower prevalence of hypertension, congestive heart failure and diabetes, which made smoking an unlikely independent predictor of death in AMI (7). Although a very large study of more than 500 000 cases of AMI could not entirely explain the lower in-hospital mortality of smokers by the measured covariates (8), it is quite clear that smoking does not offer protection in the context of AMI, but rather that smokers suffer myocardial infarction at a significantly younger age than non-smokers with an otherwise similar risk-adjusted prognosis (4-7, 9, 10).
The content of this article reflects the personal opinion of the author/s and is not necessarily the official position of the European Society of Cardiology.
Conclusion:
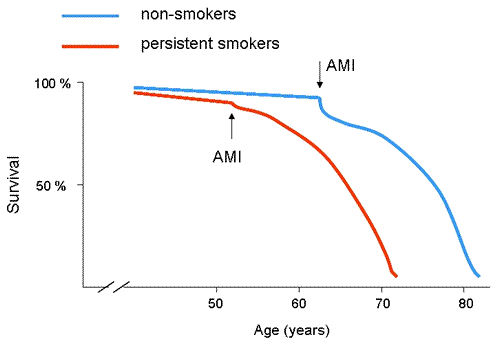
The use of terms such as “smoker’s paradox” or “paradoxically beneficial effects of smoking on the early outcome of AMI” should be avoided, especially because they are misleading to the lay public. In fact, stopping smoking after AMI reduces the risk of death in the subsequent 2 – 10 years by almost one half in comparison with persistent smokers: in a meta-analysis of 12 studies the combined odds ratio was 0.54 with a 95 % confidence interval of 0.46-0.62 (11). Health care professionals should continue their efforts in promoting non-smoking lifestyle and assisting in smoking cessation.


 Our mission: To reduce the burden of cardiovascular disease.
Our mission: To reduce the burden of cardiovascular disease.