Background
In 1772, William Heberden, a British physician, aptly described the features of classical angina of effort, remarking on its occurrence with exertion and prompt resolution with rest. This was later attributed to fixed obstructive coronary atherosclerotic disease and associated with dynamic ST segment depression on the electrocardiogram (ECG) during pain.
In 1959 Prinzmetal et al (1) described 32 cases of angina occurring at rest, reporting that the clinical characteristics of these patients differed to those with Heberden’s classical angina of effort since:
- The angina did not occur with exertion and exercise - stress tests were typically negative
- During pain, ST segment elevation rather than depression occurred
- The angina episodes often recurred at the same time, frequently awaking the patient from sleep
- The episodes may be associated with arrhythmias or progress on to myocardial infarction
Considering these differences, Prinzmetal coined the term "variant angina" and speculated that the condition was due to an "increased coronary tonus" or vasospasm. Since then, there have been significant advances in our understanding of this condition with the principle pathophysiologic mechanism responsible for the syndrome being occlusive spasm of an epicardial coronary artery. Consequently, provocative spasm testing has been developed to aid in its diagnosis. Despite these advances, clinicians are often unclear in the diagnosis of variant angina and this communiqué will endeavour to clarify these issues.
1. Clinical Features
Clinically, the hallmark features of variant angina include:
- Recurrent episodes of rest angina, often occurring in the early morning hours, associated with
- Transient ST segment elevation
- Prompt alleviated with short-acting nitrates
A high index of suspicion for this diagnosis must be considered in patients awakening with recurrent brief episodes of nocturnal angina, promptly relieved with sublingual nitrates. The diagnosis must also be considered in patients with recurrent rest angina associated with syncope or even cardiac arrest, since patients with variant angina may experience malignant arrhythmias during their ischaemic episodes.
Except for cigarette smoking, the conventional atherosclerotic risk factors do not appear to predispose patients to variant angina. Also in contrast to atherosclerotic disease, the condition appears to be more prevalent amongst the Japanese as compared with Caucasians (2). Whereas exercise does not typically precipitate an episode of variant angina, hyperventilation and exposure to the cold can provoke episodes.
The temporal pattern of the rest angina warrants close consideration in evaluating these patients, both in relation to its waxing and waning nature and its distinct circadian rhythm. Variant angina may remain quiescent for prolonged periods and then recur with multiple frequent episodes. During these "hot phases", stimuli that would not usually provoke an episode of variant angina, may induce an episode. The circadian nature of this disorder is also well recognised and illustrated by Yasue et al (3) who could provoke ST elevation in variant angina patients in the early morning (5-8am) but seldom when repeated in these patients in the afternoon (3-4pm).
2. Diagnostic Evaluation
The clinical history and ECG recording during a spontaneous attack are paramount in the clinical diagnosis of variant angina. However since spontaneous episodes are infrequently captured on ECG, additional investigations must be considered.
- Ambulatory ECG monitoring may be useful, particularly during a hot phase of the condition, for detecting episodes of ST segment changes as well as associated arrhythmias.
- Exercise ECG stress testing is typically negative but during the hot phase, exercise-induced spasm may occur in half of the variant angina patients (4).
- Coronary angiography is useful to assess the presence of obstructive coronary artery disease: A frequent misconception in contemporary cardiology is that variant angina should only be considered in patients with normal angiography; however Prinzmetal’s original description of the condition included patients with significant coronary artery disease, where spasm occurred on a non-critical stenosis thereby producing transient vessel occlusion and thus ischaemia associated with ST elevation that was alleviated by sublingual nitrates. Subsequent studies reported the ‘variant of the variant’ where variant angina was found to occur in patients with normal angiography (5).
- Provocative coronary spasm testing: was initially performed at the bedside with ECG monitoring alone. However following several deaths using this approach, provocative testing has primarily been undertaken during coronary angiography, where spasm can be promptly identified and treated with intracoronary nitrates if necessary. A variety of provocative stimuli have been used for spasm testing including methacholine, adrenaline (with/without propranolol), phenylephrine, serotonin, histamine, dopamine, methylergometrine and hyperventilation with TRIS buffer infusion but the two most commonly employed in contemporary practice are acetylcholine and ergonovine. Intracoronary acetylcholine is administered as incremental selective slow bolus injections into the right (25-50mcg) and left (25-100mcg) coronary arteries, frequently requiring pacing due to the transient cholinergic-induced bradycardia (6). Slow intracoronary bolus injections of 20-60mcg ergonovine into the right and left coronary arteries have been used by some clinician whilst others utilise incremental intravenous bolus injections (25-300mcg) at 5-minute intervals (4). The presence of inducible coronary spasm is assessed on the basis of chest pain, ECG changes and/or severe coronary constriction in response to the provocative stimulus.
The differential diagnoses for patients with suspected variant angina (rest pain with ST elevation) include an evolving myocardial infarct, mixed pattern angina, tako-tsubo cardiomyopathy, and coronary microvascular disorders. Although variant angina may progress on to ST elevation myocardial infarction, the former is distinguished by a history of recurrent chest pain and prompt response to nitrates. Mixed pattern angina (both exertional and rest pain) was coined by Maseri (4) and acknowledges the spectrum of coronary disorders from exertional angina due to fixed obstructive coronary artery disease to dynamic spasm as occurs with variant angina. Tako-tsubo cardiomyopathy may manifest as rest angina associated with ST elevation. Although the classical apical ballooning may distinguish it from variant angina, some investigators speculate that this curious entity is due to multivessel spasm. Coronary microvascular disorders may cause rest angina in patients with normal angiography, which may be distinguished from variant angina by excluding coronary artery spasm with provocative spasm testing. In the absence of documented ischaemia, other non-cardiac causes of rest pain (eg oesophageal spasm) need to be considered.
3. Diagnostic Criteria
Two approaches have evolved in the diagnosis of variant angina. The first is based upon Prinzmetal’s clinical criteria for diagnosing variant angina including 1) rest angina, with 2) transient ST elevation, and 3) improvement/resolution with sublingual nitrates. Many early studies utilised this clinical approach but with the advent of imaging the coronary arteries via selective angiography, the focus has moved towards the diagnosis based upon provocative spasm testing. With this later approach, the term "vasospastic angina" was coined with the following diagnostic criteria, 1) rest angina, 2) reversible ST changes (elevation or depression), and/or 3) spontaneous/provoked coronary spasm on angiography. Although these diagnostic approaches differ, there is significant agreement since validation studies have reported a 90% sensitivity and 99% specificity in the provoked spasm on angiography with the Prinzmetal clinical diagnostic criteria (7). Guidelines for the diagnosis and management of vasospastic angina have been produced by the Japanese Circulation Society (6) although these still need to be developed in other countries (8).
4. Management
The management of Prinzmetal angina focuses on:
- Avoiding predisposing factors such as smoking and preventing coronary spasm by the use of vasodilator therapies.
- Short-acting nitrates are utilised for acute episodes whereas the long-acting nitrates are used to prevent vasospastic episodes.
- The addition of calcium channel blockers to background nitrate therapy has been shown to reduce cardiac events in patients with variant angina (9).
- The potassium channel opener, nicorandil, and the rho kinase inhibitor, fasudil, have both been shown to be effective in preventing coronary spasm episodes and are useful therapies for this condition.
5. Prognosis
Variant angina may be associated with significant morbidity and mortality with infarct-free survival being 60-95% at 5 years (Figure-1). Independent determinants of infarct-free survival include the use of calcium channel blockers, extent and severity of coronary artery disease, and multivessel spasm (9). As shown in Figure-1, Caucasian variant angina patients have poorer outcomes than their Japanese counterparts, which in part may be due to the increased prevalence of coronary artery disease.
6. Conclusion
Variant angina can be readily diagnosed by clinical criteria and/or provocative spasm testing, yet it is often not considered. Given that it can have life-threatening sequelae that are preventable with readily available therapies, it is essential that clinicians are vigilant in considering this condition.
Figure 1: Long-term infarct-free survival in Japanese (9-11) (filled shapes) and Caucasian (12-15) (open shapes) patients with variant angina. Adapted from Beltrame et al (2], J Am Coll Cardiol. 1999, 33:1445.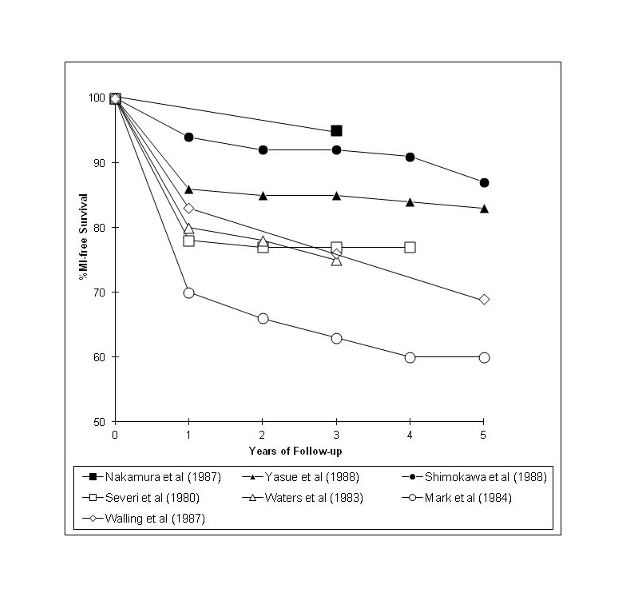


 Our mission: To reduce the burden of cardiovascular disease.
Our mission: To reduce the burden of cardiovascular disease.