Dr. Anton Sirnes represents Norway in the Council for Cardiology Practice.
He is President of the Private-practicing cardiologists' forum of Norway.
The Kingdom of Norway has 4.6 million inhabitants, a physician density of 250 inhabitants per doctor and an almost fully state-regulated health care system. There are about 200 working cardiologists, of which 30 work in private practice. Local communities are responsible for primary care. Regional health care companies manage all specialised care; they deliver the licenses and pay an income to the specialist, who is then obliged to work in his office for 37.5 hrs a week for at least 44 weeks per year. To that wage the specialist adds patients’ fees and NHS reimbursements. Yet most out-of–hospital based cardiologists only earn marginally more than general practitioners.
Health care in Norway
The Kingdom of Norway has 4.6 million inhabitants and is not a member of the EU, but collaborates extensively with EU countries through the EFTA (European Free Trade Association) agreement (1). Physicians who are licensed in Sweden or Denmark will usually be licensed in Norway without any major difficulties. A medical education and speciality credential from a European country are recognised in Norway, but there are specific national requirements which have to be fulfilled in order to get a Norwegian licence.
Norway has a physician density of 250 inhabitants per doctor, which is among the highest in Europe (2) and the total health care expenses per inhabitant are also amongst the world’s highest (table 1). The health care system in Norway is almost fully state-regulated. All citizens are members of the National Health Service system (Folketrygden) which subsidises important medication and part of the fee for Doctors' visits.
Cardiology in Norway
The speciality of cardiology in Norway is a sub-speciality in general internal medicine. To obtain credentials as a cardiologist one has to serve at least 18 months in the cardiology department of a referral hospital. There are presently 1925 recognised specialists in internal medicine, and of these 417 also have credentials as cardiologists. However, should we only take into account those under the age of 70 who are working as cardiologists, the number is about 200 for the whole of Norway. Amongst these, the number of cardiologists in private practice is between 25 and 30.
All cardiologists in private practice are automatically members of the Norwegian Medical Association and are also members of the Norwegian Society of Cardiology, but the Norwegian National Society of Cardiology has declined to form a separate group for out-of-hospital based cardiologists. We therefore have our own organisation: PPKF (Privat Praktiserende Kardiologers Forum), which is now a member organisation of the Council for Cardiology Practice of the European Society of Cardiology. PPKF was founded as an informal group in 1993 and has had 1-3 meetings annually - usually parallel to international cardiology conferences. However, over the last few years we have also arranged our own conferences focusing on the practical application of echocardiography.
Local communities are responsible for primary care
At the first level, the local communities are responsible for primary care. Primary care physicians have obtained contracts with local communities. They get paid partly on a fixed basis according to the number of persons on their patient list and partly based on direct patient’s fees on reimbursements for consultations and procedures.
Regional Health care companies manage all specialised health care
The second level of health care, which is for all specialised health care, comprises all the hospitals and out-of-hospital free specialists, and is managed by regional health care companies. Norway is divided into four health care regions. In each region a public health care company is responsible for all the second level health care. The leaders and the board of public health care companies are appointed by the government and each regional health care company is given a limited budget to cover specialised health care – both hospitals and contract-bound specialists in private practice.
Out-of–hospital physician-specialists, such as cardiologists, are closely regulated
In theory, any cardiologist with a valid license can set up a private practice and treat patients. However, without a contract with the regional health care company patients would have to pay the whole fee from their own pocket.
To work in an out-of-hospital based specialist practice one has to obtain a contract with the regional health care company, which can decide upon the geographic location of the office. There are only a limited number of such contracts available. Currently there are about 26 concessions given out to cardiologists in the whole of Norway. Historically, such contracts were given out to those who were already established in private specialist practice in 1995. New contracts are very rare.
When a specialist retires, the contract is made available by an announcement from the regional health care company. The physician who obtains the contract has to pay the previous owner a sum for equipment and good-will. There is also a special arrangement which enables a specialist aged over 60 to gradually include a partner over a transition period of 5 years. Once aged 70, the specialist looses the contract with the regional health care company and privileges with respect to reimbursements from the National Health Service.
Having obtained a contract, the specialist is granted a fixed yearly income of approximately €117.400 (typically for large practice like cardiology) paid by the regional health care company. The specialist is then obliged to work in his office for 37.5 hrs a week for at least 44 weeks per year. Opening hours for patients must be 80% of this time. The license cannot be shared with other doctors. The license allows for fellow cardiologists to replace the owner of the license on a temporary basis, for reasons such as illness or education.
Obtaining a contract with the regional health care company enables the physician to also obtain a contract with the NHS. This contract makes it possible to obtain reimbursements for each consultation and for procedures performed according to a national scheme (“Normaltariffen”), which is negotiated yearly.
Access to the cardiologist for the public is not free. The general practitioner has a gate-keeper function and has to write a letter of referral to the specialist. In order to benefit from the reimbursement, a copy of this letter is required. For chronic diseases the reimbursement for referral can be obtained once yearly without a new referral letter.
The current NHS rate of reimbursement for a cardiologist in private practice is presented in table 2. When the amount a patient has paid for physicians fees and medication (up to about €40 per prescription) exceeds €210, the patient and his family get as “free card” for the rest of the year, covering all physicians’ fees and expenses for important medication.
With three sources of income, the fixed sum from the regional health care company, the patients’ fees and the NHS reimbursement, the cardiologist has to pay out for office rent, expensive equipment, wages to nurses and secretaries and so on. Before income tax (in Norway usually up to 55% of the total income), most out-of-hospital based cardiologists will have an annual income between €130 000 – €200 000. This is only marginally more than most general practitioners.
Typically a cardiologist in a private practice has 1700-2500 consultations per year, will see 800-1200 new patients and perform around 700 -1200 echocardiographic examinations and 600-900 exercise ECGs.
Table 1. Consultation fees in Norway as of 2007. (Numbers in Euros) 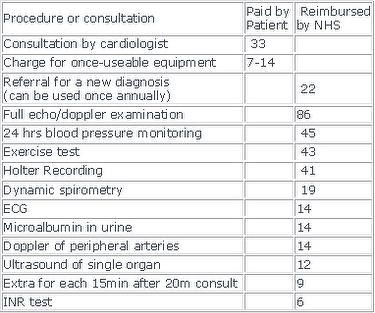
Private internal medicine practice can also charge these fees with the exception of echocardiography.
Table 2.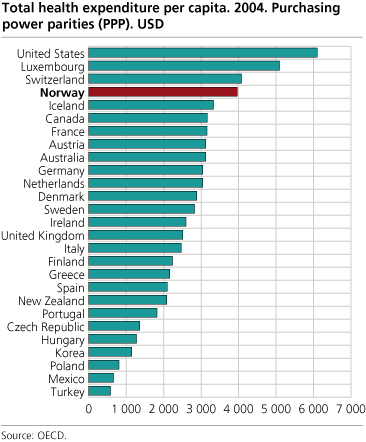
1 - European Free Trade Association:
http://www.efta.int/
2 - Statistics and Research on physicians in Norway in English: http://www.legeforeningen.no

 Our mission: To reduce the burden of cardiovascular disease.
Our mission: To reduce the burden of cardiovascular disease.