Mitral regurgitation (MR) is a frequent complication during and after the acute phase of a Q-wave acute myocardial infarction (AMI) and it is a predictor of long-term cardiovascular mortality (1-6). Very recent studies have demonstrated its prognostic implication after a non-Q wave AMI (7), the role of the existence of MR previous to an AMI (8) and its prognostic importance after a non-ST segment elevation acute coronary syndrome (NSTSEACS) (9).
Functional MR occurs with a structurally normal valve as a result of an altered force balance on the mitral leaflets (10). Its causal mechanisms have been studied in the acute and in the chronic stage after a Q-wave AMI. They include ischemia or scar at the level of the papillary muscles, annulus dilatation, change in the ventricular geometry causing tethering of the mitral leaflets and systolic dysfunction (5-10). Nevertheless, factors involved in the development of MR after NSTSEACS are still not well understood.
In a recent study, three hundred consecutive patients who were admitted to the Coronary Care Unit for a first NSTSEACS were evaluated and followed-up. Every patient had an established diagnosis of NSTSEACS based on the European Society of Cardiology criteria (11). All patients underwent a complete echocardiographic study before hospital discharge that included a specific evaluation of the mitral valve anatomy and function. The presence and degree of MR was evaluated using PISA method and a validated nomogram for semiquantitative estimation (12,13).
The main results of this study showed that a higher age and a lower ejection fraction are independent markers of MR development in this clinical scenario, probably due to the left ventricular remodelling that they cause. Patients were followed-up for a median time of 431 days. Survival curves showed that long-term outcome depends on MR presence and severity (figure). Furthermore, MR was found as a long-term independent predictor of bad outcome.
In this work, patients with a NSTSEACS and functional MR have larger left ventricular systolic diameters, as well as lower left ventricular ejection fractions. Hibernated or stunned myocardium might produce left ventricular remodelling in hearts with no transmural necrosis and the progressive change in LV size and shape might lead to the development of MR (7). It has been described that left ventricular dysfunction resulting from viable hibernating but recoverable myocardium has a better prognosis when revascularisation is performed and that an improvement of myocardial performance and reversal of dilatation decreases MR after surgical revascularisation (14,15). In this study (9), the development of MR was associated with a worse long-term outcome but it is not associated to a worse in-hospital outcome. This finding could be due to the fact that the deleterious action of post-NSTSEACS MR is based on a progressive left ventricular remodelling that develops over time. The results of the present study contrast with the results of a previous work (7) in which the presence of MR did not add any independent prognostic significance in the setting of non-Q wave AMI. Nevertheless, one must note that the population in that study was significantly smaller and the definition used for inclusion was the old definition of non-Q wave acute myocardial infarction instead the new definition of NSTSEACS.
Nevertheless, this study has some limitations. Pre-AMI MR is a recently described prognostic factor (8). It is not possible to make sure that MR was not present before the index NSTSEACS but it is very difficult to distinguish between pre-existing MR and new-onset MR. Furthermore, the morphology of the mitral valve was not specifically assessed or quantified in this work. Thus, the diagnosis of functional MR was performed excluding those patients with structural alterations at the level of the mitral leaflets or mitral subvalvular apparatus, following the methods used in previous reference papers (6).
CONCLUSIONS
Summarising, we can say that functional MR is a frequent complication after both, a Q-wave AMI and after a NSTSEACS. Furthermore, after any type of acute coronary syndrome, the presence and degree of MR adds long-term prognostic significance to other known negative factors. Thus, the presence of MR should be specifically assessed in every patient after a Q-wave AMI and also after a NSTSECAS. Nevertheless, until now, no therapeutic management has demonstrated a better outcome in this type of patients. Thus, further research is needed in this field.
Figure: Long-term outcome survival curves.
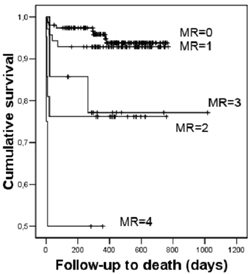
Figure legends :
MR: mitral regurgitation. 0: absence of MR or trace MR; 1: mild MR; 2= mild to moderate MR; 3: moderate MR; 4: severe MR. (adapted from Pérez de Isla L et al. Prognostic significance of functional mitral regurgitation after a first non-ST-segment elevation acute coronary síndrome. Eur Heart J 2006 27: 2655-2660).
The content of this article reflects the personal opinion of the author/s and is not necessarily the official position of the European Society of Cardiology.



 Our mission: To reduce the burden of cardiovascular disease.
Our mission: To reduce the burden of cardiovascular disease.