Background
Awareness that cardiovascular disease is a leading cause of premature death, most often manifested as coronary artery disease - is spreading. (1,2)
Awareness that peripheral arterial disease (PAD) - defined as an ankle-brachial ratio of 0.9 or when patient has been previously revascularised with surgery or transluminal angioplasty - is a significant health burden however is not, even though 10% of the general population, 20% of those above 70 years and 30% of diabetics over 50 have PAD. (3,4)
During surgery, these patients are at double the risk of cardiovascular mortality and major artery coronary events (MACE) because PAD usually comes with CAD, and vice versa. Indeed the systemic atherosclerotic process is the most common aetiology for both PAD and CAD. (5)
Endovascular therapy angioplasty also incurs a high risk of adverse cardiovascular outcome.
Pre-operative identification and treatment of cardiovascular risk factors is vital to reduce this risk; through. Appropriate interventions, investigations and drugs are detailed here.
1 - Interventions
Peripheral artery disease affects areas of the vascular bed: the carotid, lower extremity - these two being the most common - the upper limb, mesenteric or renal arteries. Whatever the area, the presence of PAD in one territory should prompt investigation for PAD elsewhere and also trigger a search for CAD (6).
The vascular surgeon, at times with the interventional radiologist, will make the determination of each individual case according to the following framework for intervention:
- Carotid endarterectomy - or endovascular carotid stenting in higher-risk patients - is recommended or considered in patients with:
A - Symptomatic carotid artery disease, recent stroke/TIA (<6 months) and >70% stenosis in the internal carotid artery, ideally also within 2 weeks of symptom onset).
B - Symptomatic patients with 50-69% stenosis
C - Asymptomatic patients with 60-99% stenosis. - Bypass surgery or endovascular intervention following an unsuccessful trial of risk factor control and medical therapy with aspirin and a statin.
- Endovascular therapy based on imaging for chronic lower extremity disease usually manifesting as intermittent claudication often with concomitant CAD.
The cardiologist should assess abnormal angiograms (in one study over 90% of patients with PAD had abnormal angiograms) and should assess: (7)
- Perioperative risk of cardiovascular adverse events - mortality, myocardial infarction, pulmonary oedema, ventricular arrhythmia and relevant future long-term cardiovascular prognosis.
- Clinical features in the patient's history which might suggest underlying CAD, including anginal symptoms, dyspnoea, risk factors (diabetes, hypertension, hyperlipidaemia, smoking, family history).
- Adverse signs on clinical examination (evidence of pulmonary congestion, cardiac murmurs etc.
Standard 12-lead ECG should be obtained in all patients (class IB recommendation). - Resting ECG abnormalities: they are predictive of cardiovascular mortality. (8)
The following conditions should be immediately dealt with prior to any or further PAD surgery:
- Unstable cardiac conditions (acute coronary syndrome, decompensated heart failure or significant valvular heart disease for example) or clinical features suggestive of CAD based on clinical history, examination and resting ECG.
If however, there are no concerning features based on these initial screening tests, we recommend that the patient proceed to surgery as planned with no further evaluation.
Fig.1 Management flowchart for PAD patients referred for pre-operative cardiovascular assessment.
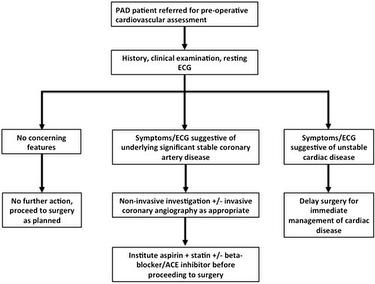
2 - Investigations
According to the 2014 ESC/ESA Guidelines on non-cardiac surgery: cardiovascular assessment and management, routine echocardiography and or functional testing is recommended only if patient has at least two among the following risk factors: Ischemic heart disease, heart failure, stroke or transient ischemic stroke, renal dysfunction or diabetes requiring insulin therapy.
Echocardiography
Pre-operative resting echocardiography can identify 1) significant valvular lesions and/or 2) severe left ventricular dysfunction in patients with:
- A cardiac murmur or a sign of heart failure
- High-risk and no symptoms (class IIa recommendation, level C). (9)
Functional testing
Exercise ECG
In patients in whom history is suggestive of angina, exercise treadmill testing (ETT) is a first-line screening tool for assessment of ischemia. Indeed, in a group of patients due to undergo vascular surgery, ETT showed acceptable diagnostic accuracy, similar to that of the general population (sensitivity 74%, specificity 69%). (10)
However stress echocardiography, nuclear imaging or stress CMR (see below), depending on availability, would be recommended when 1) patients with limited exercise tolerance due to limb claudication are unable to reach optimal exercise stress 2) resting ECG abnormalities cause difficulty in ETT interpretation.
Stress echocardiography
Stress echocardiography is most commonly administered using dobutamine or dipyridamole given the limited exercise tolerance of patients with PAD.
Extremely good prognosis is signaled if it is negative. The presence of an inducible wall motion abnormality is a relatively poor predictor of peri-operative MACE (positive predictive value 25-45%). In this group of patients, dobutamine may have a slightly higher sensitivity than dipyridamole.
Nuclear imaging
Nuclear scintigraphy is well validated as a pre-operative risk stratification tool in patients with PAD. Its predictive power is similar to dipyridamole stress echocardiography. (11)
As with stress echocardiography, the negative predictive value of nuclear imaging is extremely high.
Stress cardiovascular magnetic resonance
Stress magnetic resonance imaging using dobutamine or adenosine has excellent diagnostic accuracy for identification of significant ischaemia, however there are not any data as yet on its value in pre-operative risk stratification.
Computerised tomography coronary angiography
Multislice computerised tomography (MDCT) coronary angiography defines coronary anatomy non-invasively. Its sensitivity for diagnosis of significant coronary stenoses is very high and may be useful in patients with inconclusive functional stress tests. (12, 13) Nevertheless, given the prevalence of CAD in patients with PAD, these patients often have a higher pre-test probability. Current ESC guidelines for investigation of stable angina recommend coronary CT in patients with 15-50% (i.e. low-intermediate) pre-test probability. (14) Despite this, the absence of significant stenosis seen using coronary CT has been shown to have good prognostic value in predicting peri-operative mortality in patients at intermediate risk but has not yet been evaluated in a high-risk cohort.
Invasive coronary angiography
Current guidance recommends pre-operative invasive coronary angiography in patients with PAD and acute coronary syndromes or angina despite optimal medical therapy i.e. similar to current indications in the general population.
In high-risk patients without any cardiac symptoms, pre-operative invasive coronary angiography is one option, however this should not delay any urgent PAD surgery, which should always be carried out first. It is important to note that there is, at best, conflicting evidence to suggest any mortality benefit with a routine pre-operative invasive strategy. (15-17) Furthermore, the requirement of dual anti-platelet therapy post-stenting may delay surgery, which may not be ideal.
In our opinion, patients with a clear history of angina and documented ischaemia or CT evidence of severe stenosis should undergo pre-operative angiography with a view to percutaneous coronary intervention. We would not recommend routine angiography of asymptomatic patients without documented ischemia.
3 - Drugs
Beta-blockers
Among the most studied group of drugs in this area are beta-blockers. Until 2011, the guidelines were clear – beta-blockers, initiated between 7 to 30 days prior to operation in patients undergoing PAD surgery.
The DECREASE trial drove the evidence for this strategy, the methods of which have been called into question since and have lead both the ESC and the American societies to rewrite their guidelines. (18)
A meta-analysis published in 2011 without the DECREASE trials suggests that while pre-operative beta-blockers may reduce risk of non-fatal MI (by 27%), there was a 27% increase in all-cause mortality, and higher risk of stroke and hypotension. (19) The ESC has since recommended an individualised approach to pre-operative beta-blockade over routine and the latest guidelines advocate their use only when there are other indications, such as heart failure of ischaemic coronary disease. We would add that most patients should not routinely receive a beta-blocker and normal cardiological indications should be followed for patients with reduced left ventricular ejection fraction, atrial fibrillation with a fast ventricular rate and stable angina.
Other drugs
Pre-operative statins are recommended. (20-22) These should also be continued during the operative period to avoid a rebound effect that can occur with their discontinuation.
ACE-inhibitors (or angiotensin receptor antagonists) should be started in patients noted to have left ventricular systolic dysfunction pre-operatively (and surgery delayed to allow their initiation, if possible).
The key point regarding any other drugs is that the patient’s pre-operative regime should be continued during the operative period.
Conclusions
Patients undergoing surgery for PAD are at high risk of peri-operative adverse cardiac events, primarily due to the systemic atherosclerotic process.
- All patients should undergo detailed clinical history taking, examination and resting ECG to determine baseline cardiac risk.
- Further investigation and management should be directed based on this initial evaluation. Our suggestion for management is summarised in figure 1.
- In asymptomatic patients with no significant ECG abnormalities, no further investigation is required and they can proceed to surgery.
- Patients with unstable cardiac conditions such as MI or heart failure should have these dealt with immediately.
- In other patients, it is important to continue routine pre-operative cardiac medications, with initiation of statins for those suspected to have some cardiovascular risk (in practice, essentially all patients with PAD) and ACE inhibitors and beta-blockers in those with reduced left ventricular function.
- Evidence for routine use of pre-operative beta-blockers in all patients is inconclusive.


 Our mission: To reduce the burden of cardiovascular disease.
Our mission: To reduce the burden of cardiovascular disease.